OUTCOMES ANALYZER℠
Persistent, Configuration-Driven Healthcare Program Evaluation
Structured, defensible impact measurement — enhanced by intelligent, AI-assisted reporting.
Built for enterprise healthcare environments — designed to withstand finance and underwriting review.
Most reporting answers: What happened? Outcomes Analyzer answers: Did it work — and is the result durable?
Outcomes Analyzer℠ is deployable as a standalone evaluation application and can also be implemented alongside enterprise analytics infrastructure when deeper integration is required.
Evaluation Outcomes in Practice
Configuration-driven evaluation across diverse healthcare stakeholders.
Challenge
A large regional health plan needed to demonstrate measurable ROI across multiple healthcare initiatives for employer groups. Existing evaluations were episodic, manually constructed, and difficult to reproduce consistently.
Methodology varied by analyst, cohort definitions shifted over time, and results were difficult to defend under finance or underwriting review.
Case Study 1 — Health Plan
Solution
Outcomes Analyzer established a standardized matched-cohort evaluation framework using integrated medical, pharmacy, eligibility, and participation data.
Evaluations were configuration-driven and recalculated as new claims matured — preserving cohort integrity and aligning financial outputs with employer reporting cycles.
Results
Standardized, reproducible ROI measurement across employer groups
Reduced analyst time rebuilding one-off studies
Clear cohort validation and documentation suitable for finance-level review
Business Impact
The health plan strengthened employer and consultant conversations through defensible, claims-based impact measurement.
Consistent methodology improved renewal positioning, supported retention discussions, and differentiated the plan in competitive bids.
Challenge
A maternity support solution provider reported a short-term 1.8:1 ROI after two months — attractive, but vulnerable to scrutiny. The evaluation window was limited, baseline risk differences were unaccounted for, and neonatal costs were excluded.
Consultants, actuaries, and CFOs questioned durability, representativeness, and attribution.
Case Study 2 — Point Solution Provider
Solution
The vendor commissioned a longitudinal, claims-based evaluation using matched control methodology.
The analysis extended to six months, incorporated maternal and neonatal costs, and applied risk adjustment across key variables including maternal age, OB risk scores, and delivery type.
Client-specific reporting was produced alongside aggregate results.
Results
Short-term savings confirmed but flattened over time
Impact varied meaningfully by delivery type and risk mix
Low-risk deliveries sustained cost reductions
Higher-risk C-sections showed limited net savings
Uniform ROI was revealed to be heterogeneous across segments and time horizons.
Business Impact
Replacing a single headline ROI with segmented, risk-adjusted reporting shifted the vendor from defensive justification to credible dialogue.
Renewal positioning strengthened, buyer trust improved, and internal insight informed product strategy.
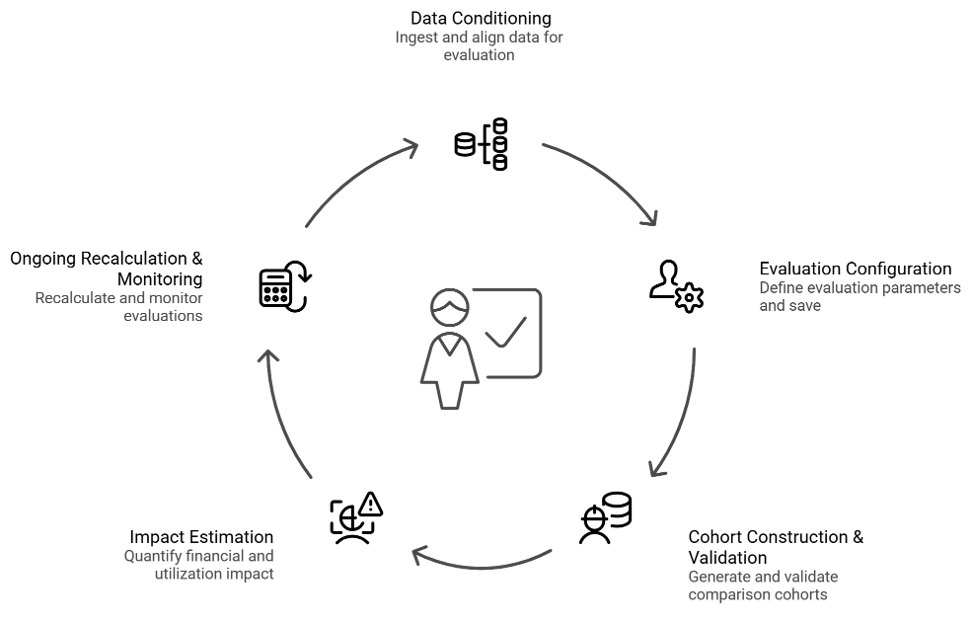
How Outcomes Analyzer Works
Outcomes Analyzer formalizes cohort-based evaluation within governed configurations — ensuring every reported result is traceable, reproducible, and aligned to defined methodology. Each evaluation is defined, saved, and version-controlled. As new claims mature and refresh, results recalculate within the same structured configuration, preserving comparability across reporting periods.
Intelligent Interaction & Reporting
Outcomes Analyzer℠ integrates AI-assisted interaction within its governed evaluation framework — enabling authorized users to explore structured results while preserving methodological integrity.
Users can:
Interrogate program impact across defined refresh cycles
Generate executive-ready summaries from saved configurations
Examine cohort stability and financial impact diagnostics
Produce renewal-ready reporting grounded in validated outputs
The AI interface enhances accessibility and interpretation; it does not modify statistical methodology. Every output remains reproducible, auditable, and governed within enterprise-defined methodological standards.
Transparent Configuration. Defensible Results.
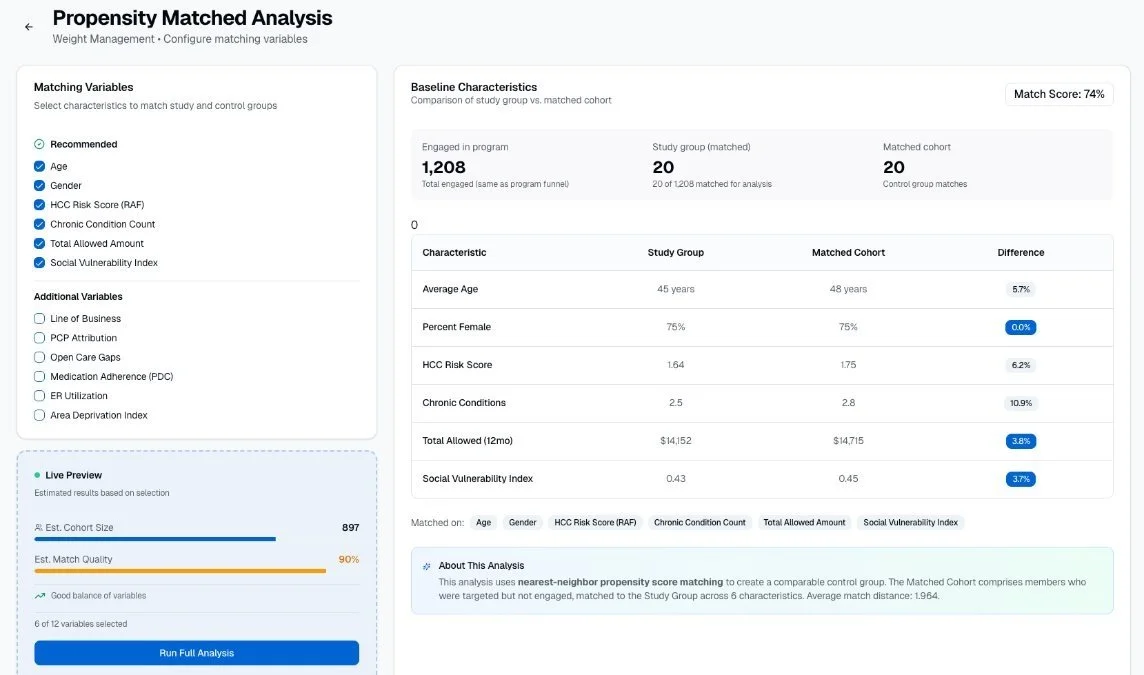
Outcomes Analyzer formalizes cohort-based evaluation through structured configuration and visible matching logic. Study and control groups are defined, preserved, and recalculated consistently across reporting cycles.
Matching variables, baseline balance, and financial impact calculations remain transparent — enabling reproducible, audit-ready program evaluation.
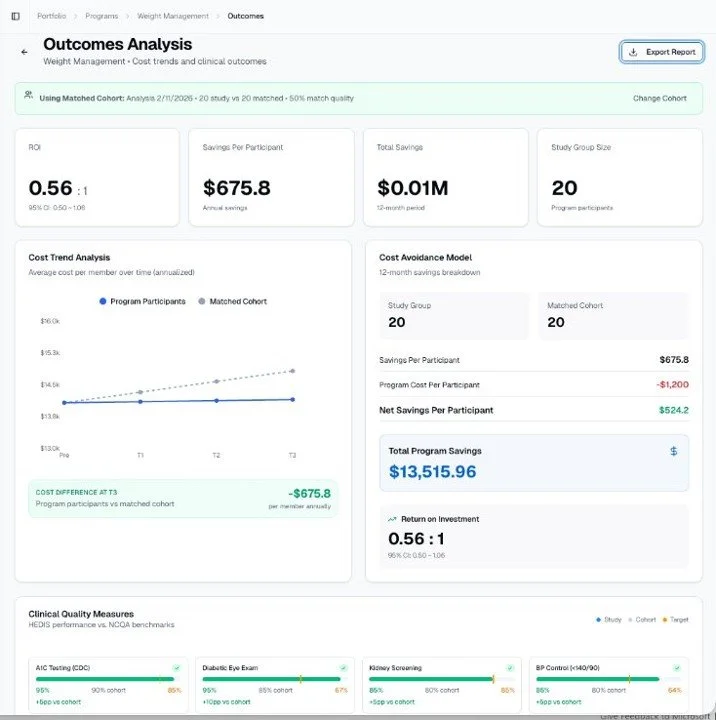
Configuration-driven matching with visible baseline balance and match quality scoring.
Structured impact reporting with financial, utilization, and clinical quality alignment across defined intervals.
See the Evaluation Framework in Practice
Explore how configuration-driven evaluation produces durable, audit-ready outputs.
Deployment & Operating Model
Outcomes Analyzer operates within enterprise data environments and established governance frameworks.
Embedded Deployment (Preferred)
Outcomes Analyzer can be deployed within a payer or employer’s existing data environment, leveraging internal data warehouses, security protocols, and access controls. This model minimizes data movement and aligns with enterprise compliance standards.
Managed Deployment (Optional)
Where embedded deployment is not feasible, a secure managed model can support structured evaluation using the same workflow and methodology, with clearly defined data governance and refresh cadence.
Refresh Cadence
Evaluations are typically recalculated on a quarterly basis, aligned with data maturity and reporting cycles. Saved configurations ensure consistency across evaluation periods and enable longitudinal monitoring.
Designed for Enterprise Healthcare Accountability
Health Plans & Payers
Standardize and scale program evaluation across employer groups and point solutions within a governed enterprise framework.
Outcomes Analyzer enables internal analytics teams to configure, validate, and refresh evaluations centrally — while distributing structured, defensible impact results across hundreds of employer accounts. Cohort comparability, financial logic, and reporting cadence remain consistent across the portfolio.
Employers
Institutionalize program evaluation as an ongoing capability rather than a one-time study.
Outcomes Analyzer allows employers to define impact methodologies once, preserve configuration integrity, and monitor performance across refresh cycles — supporting renewal decisions, vendor accountability, and executive reporting with audit-ready outputs.
Point Solution Providers
Demonstrate program performance across multiple client populations using a consistent, statistically valid framework.
Outcomes Analyzer enables providers to monitor impact longitudinally, preserve evaluation integrity across client environments, and generate renewal-ready reporting grounded in structured cohort methodology.